Healthcare Innovation: Reframe Problems to Seize New Opportunity
Alongside headline-worthy turmoil over healthcare and insurance, the medical device and technology industry itself is undergoing transformative change. How can medical device companies break through the seemingly endless barriers to create new value and thrive? One proven strategy lies in reframing problems to see new opportunities and deliver healthcare innovation.
Let’s be honest: Creating the next breakthrough medical device design, service or solutions in healthcare has never been easy.
With highly regulated environments and long development timelines, increasing complexity, numerous competing stakeholders, and a hefty responsibility to do no harm, the development of medical devices designed to cure, heal or help is already hard. Today, however, manufacturers and designers face a myriad of additional burdens to deliver healthcare innovation, from an industry in flux to intense competition and increasing costs, to a multitude of obstacles that prevent medical device companies from effectively collaborating with the principal healthcare stakeholders.
What can we do? Turn the tables.
In practical terms, we speak of it like this: “reframing a problem to recognize the opportunities within.” From our experience partnering with leading healthcare companies, the following five problems are among the most common the industry faces. We’ve given each of them a nod, and you some practical advice on how to turn them into possibility—along with examples of medical device product development companies reaping the benefits of challenging the status quo and reframing problems into opportunities for new value creation.
Problem #1: The Vagaries of “Value”
One of the biggest internal shifts in the healthcare industry in the recent past has been and continues to be the systemic move from “fee-for-service” care to “value-based” care. Practically speaking, “fee-for-service” was an easier revenue and innovation model to understand. Things cost what they cost, and businesses were reimbursed for procedures based in part on the number of them performed. The path from product to outcome was clear—making the measurement of effectiveness straightforward. In the value-based world, success is tied more closely to outcomes—how much a patient’s health has improved. As a result of this shift, many medical device companies find themselves stuck at key points in the innovation process, grappling with defining “What is the value? Who evaluates the value? And, “How do we measure it?”
The challenge is: If you don’t understand what constitutes value for your stakeholders, how can you create healthcare innovation for them and measure success? It’s difficult for a product developer to generate data on how their work affects not only direct treatment but the downstream healthcare supply chain in the post-fee-for-service universe; meaning that determining the true value of an innovation is a challenging proposition.
Reframe! Understand Value Through a Multi-Stakeholder Lens
One strategy for understanding the multi-faceted definition of “value” is to ask better questions from the key stakeholders (e.g., users, decision makers, influencers, etc.) in your healthcare ecosystem. Understanding value drivers from the perspective of all the different stakeholders give healthcare innovation teams a holistic picture of what “value” really is and is not. To the procurement stakeholder, the value is equated with cost containment and reduced risk. To a surgeon, the value might be associated with efficiency, performance, and comfort – regardless of cost. What do the nurses want? Hospital Administrators? Insurance Payors? You need to know the answers to innovate in ways that make a true, sustainable impact.
As the complexity of problems in the healthcare system increases, healthcare innovation teams need to see differently and ask questions that widen and deepen their collective understanding. Adopting a holistic, multi-stakeholder lens enables teams to hear what’s needed, understand the true problem to solve, and determine what constitutes value. This can ultimately lead towards service-based solutions that deliver true value to key stakeholders and may be the answer to “How do we innovate to succeed?” According to Design Continuum, “To deliver effective value-based outcomes, device manufacturers must move beyond product-centric business models and use service design to create more comprehensive healthcare experiences for the future. Service design goes further than business process optimization; it looks beyond the status quo to define a future vision, one that may be radically different from current care delivery models.”
The bottom line is that a complex and shifting measurement of success deserves a mutable and forward-looking solution. Think of it like this: If the benchmark for success has moved from “How a knee surgery was performed,” to “How the quality knee function was regained,” it’s also relevant for medical device companies to move from “I make a product,” to “I create a solution” that generates distinctive and meaningful value for all stakeholders.
Results! Philips Healthcare – Consulting Services & Healthcare Solutions
Philips Healthcare is leveraging its design and innovation consulting practice to provide a unique twist on the trend of medical technology companies expanding their reach by transforming into value-added service and solution providers. Like other device makers, Philips tasks its designers with giving a consistent look and feel to its family of products. But they recently challenged the organization to think bigger and explore how Philips might be able to create high-value services and solutions for its healthcare partners. Among other big questions, Philips has asked, “How might we help our partners optimize and improve the experience of an imaging suite? Maybe by designing an emergency room? A hospital department? An entire hospital?”
The Philips Ambient Experience team did just that for Florida Hospital for Children’s Emergency Department, using extensive experience assessments that tapped parents and staff to design a new pediatric emergency department. It features eight patient rooms, a triage room, children’s play and waiting areas, and has helped the hospital’s patient and family satisfaction scores rocket from the bottom 10 percent in the nation to the top 10. The emergency department is now ranked as one of the best in the nation, and employee morale has soared.
Problem #2: Intense Competition and Increasing Cost Pressures
The Operating Room (OR) is pretty crowded these days, with lots of medical technology companies competing for fixed amounts of contracts and cases. Additionally, in some markets, the patient population isn’t growing—or is even declining, owing to advances in technology.
When companies solely focus on creating products within their base business, they lock themselves into competing with others in a race-to-the-bottom on pricing—or inadvertently prevent themselves from realizing other healthcare innovation opportunities for creating value in plain sight. In some cases, the surgical site is a circle only a few feet wide. What if you broadened your perspective to include the OR experience…or even to the entire stakeholder journey across the continuum of care, what other healthcare innovation opportunities might you see?
Reframe! See Beyond the Boundaries of Your Current Business to Create New Value
Medical technology companies could take a page out of the innovation playbook in analogous industries and look across the entire stakeholder journey to uncover new pain points, identifying new opportunities and creating value. The key is looking beyond that one moment of care or interaction with the patient or physician to all the moments that happen as a result. Some good questions to ask: Where could a company create value prior to surgery? What’s needed once a patient leaves the OR? Once they leave the hospital? What might be needed as they embark upon, or finish their in-home therapy?
Results! Stryker JointCOACH
Medical device company Stryker widened its lens beyond the operating table and expanded it across the entire patient journey to create JointCOACH—a web-based communication platform that enables joint replacement patients to communicate by computer or smart phone with their hospital care team, from scheduling a surgery to 90 days of post-operative care after discharge. It includes modules for pre-op preparation, clinical protocols, information about medications and pain control, and recovery and rehabilitation activities, all delivered at key intervals. It also requires interactivity; ensuring patients remain involved in their care and communicating with their doctors.
It’s a personal spin on care that benefits patients, key stakeholders, and the organization. Physicians (and Stryker) gain a way to measure product success long after the patient has been wheeled out of the hospital, as well as assurance that they’re complying with post-op recommendations. Patients felt connected and cared for in the face of an often-overwhelming procedure, and in control of the massive amounts of information delivered to them by physicians, nurses, insurance payers, and hospital administrators.
Problem #3: Patient Empowerment and Rising Expectations
Of all the stakeholders considered in the creation of a new medical device or solution, the patient is the one who’s most often overlooked. Many hospital administrators only believe that their actual customers are the physicians who bring them the patient, not the patients themselves. Patients, however, are savvier than ever and understand the world of brand and customer service, design, and delivery quite well. They also have an unprecedented amount of control over their choices—of hospitals, procedures, physicians and even products like implants and drugs and therapies. As a result, consumer products have conditioned them to an experience level that the healthcare industry can no longer ignore.
At the same time, patients are also paying more out of their own pockets for procedures (costs that would have previously been all but invisible inside of insurance premiums). If we know anything, we know that the opening of wallets portends the raising of expectations. Further, the field of choice is broadening. According to the Christensen Institute, “In healthcare, consumer choices to address a job are not limited to specific products or services in one sector. Hospitals not only compete against retail clinics and new prescription medications but also with health food stores, gyms, and personal discipline.”
The bar has been raised. How can medical device companies and other healthcare innovators rise to the expectation of those on their operating tables?
Reframe! Adopt a Patient-Centered Mindset
Given the current demand for more patient-centered products and services, design thinking is now a core competency that, when employed, can set medical technology companies apart and deliver healthcare innovation.
This is a story about putting user experience at the forefront of design in order to communicate emotionally—not simply empirically. It’s something that requires a shift in thinking for companies who typically depend on hard data to make decisions. Patient empathy is key, and medical device companies need to flip the script, asking how the quality of life for patients can be improved, not just how the disease might be treated or cured. It’s been said a thousand times: “It’s important to treat the patient, not just the disease.”
The way forward is to consider the patient as co-creator and end user. According to Metropolis, as a “partner, professional and shared decision maker. Only when we view the experience through the patient’s eyes, shall we understand how to advance healthcare environments.”
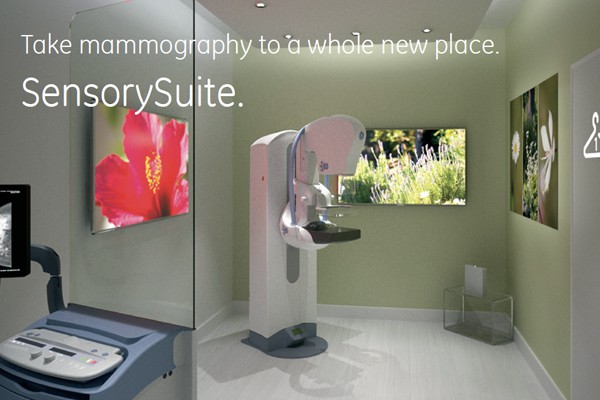
Results! GE Healthcare Sensory Suite
When re-thinking its mammography experience, GE turned to its patients—women—for guidance. Through contextual research with patients, GE found that mammography is an often-feared, much-maligned procedure that is perceived as at best a hassle and at worst a painful experience. As a result, many women forego the vital test altogether (One in every four women avoid mammograms because of worry and fear.) Armed with this information, GE designed an exam machine that distracts patients from feelings of anxiety and discomfort by offering them a personalized, self-controlled environment of soothing sights, sounds, and smells.
During the procedure, patients can control ambient room lighting, soundscapes, and soothing smells, but the real genius of this innovation might come from a large amount of preparation and pre-information patients are given before coming in for their procedure. Before the exam, women can view a demonstration online, and then play with their environment choices while waiting, ensuring they’re well prepared before ever entering the exam room.
Problem #4: Collaboration Barriers & Long Innovation Cycles
One of the best ways for medical device companies to ensure they’re innovating in ways meaningful to the medical community is to collaborate with those who know the field best: surgeons and physicians. Again, however, this is not easy. Aside from the Sunshine Act’s tight regulations on financial relationships between medical professionals and medical device companies, surgeons are also time-poor, often have apprehensions about conflict of interest, or are even in some cases prohibited by their hospitals from collaborating in research.
This is limiting, but so is the fact that most physicians are often risk averse and unenthusiastic about trying something new and unproven. For healthcare innovation, it’s a catch-22.
Reframe! Co-Create to Create New Value
We recommend that medical device companies develop and employ new collaboration and co-creation models that address challenges from multiple perspectives and collectively drive healthcare innovation across stakeholder groups and business functions.
With regard to professionals within the medical industry, this involves shifting the perspectives of physicians and other stakeholders who are willing to partner in collaboration, putting the focus on patients, their suffering and what’s at stake. Think human to human (H2H): Court motivation designed to drive social action from people driven to help and heal. HBR adapts economist and sociologist Max Weber’s principles for healthcare as such, “…shared purpose, self-interest, respect, and tradition. Leaders can use these levers to earn doctors buy in and bring about the change the system so urgently needs.”
Secondly, medical device companies can find help outside the walls of their industry, by employing design, research, and medical ethnography experts with experience in other sectors for a powerful perspective shift. According to KPMG, “Medical device companies can meet their future challenges by strengthening their abilities to complement internal capabilities with external resources and suppliers, foster cross-functional knowledge management, develop close partnerships in local markets, leverage data as competitive advantage through predictive analytics.”
Results! Johnson & Johnson Global Innovation Center
At more than 130 years old, Johnson & Johnson has taken its Global Innovation Center’s tagline, “creating new healthcare solutions never gets old” with a new approach to partnering aimed at advancing early stage healthcare innovation. Within regionally based centers in Boston, California, London and Shanghai, teams of J&J science and business experts collaborate with a myriad of innovators big and small, inside the medical field and outside, to convert scientific advances into healthcare solutions.
Their philosophy: Partner where the revolutions are happening. By working with scientists and entrepreneurs at universities, academic institutes, and start-up biotech companies, and by employing collaborative and flexible deal structures, J&J aims to identify and invest in a wide variety of pre-clinical proof of concept innovations.
Problem #5: Overcoming Short-Term Thinking
Consider this last one a bit of a warning. The healthcare industry is changing, has changed, and will change again. If medical device companies focus too tightly on their current businesses, current trends or current risks, they may find themselves stuck in incremental, short-term thinking—and that is not the stuff of transformational change (or sustained success).
Reframe! Develop Foresight To Illuminate Future Growth Opportunities
Medical device companies have a distinct need to understand how healthcare might evolve over the next decade (and beyond) to ensure relevancy and the ability to continually add value. Unfortunately, one thing no one’s invented yet is a working crystal ball.
There are some tactics and due diligence that can help you achieve healthcare innovation success, however:
– Be on top of the trend. Companies can work too closely to track and monitor economic, political, societal and technology trends in various industries to get hints about possible futures.
– Medical device companies should invest in forecasting and scenario planning to prepare for not just the most likely futures, but also multiple possibilities. A great question to search for the answer to What is likely to disrupt your current business?
– Get aligned. Develop a common, internal vision of these possible, uncertain industry futures, and then evaluate and determine what to do differently if particular scenarios come to fruition.
– Know your strengths. Understand where current strategies are robust enough to survive and thrive in alternative future states.
– Know the signs. Monitor your business environment for early signals and indicators of a particular scenario unfolding.
Conclusion
As we’ve mentioned, the healthcare and medical device industries are changing. Constant change is now the norm. The key to sustained healthcare innovation success: own the idea that complexity will always lie around every corner, and find the good in every potentially challenging turn in the road.
It’s all about perspective. Where there is a problem…there is always an opportunity. Find yours.